The Howard Chen Lab
Molecular Imaging of Cardiac Autophagy in vivo
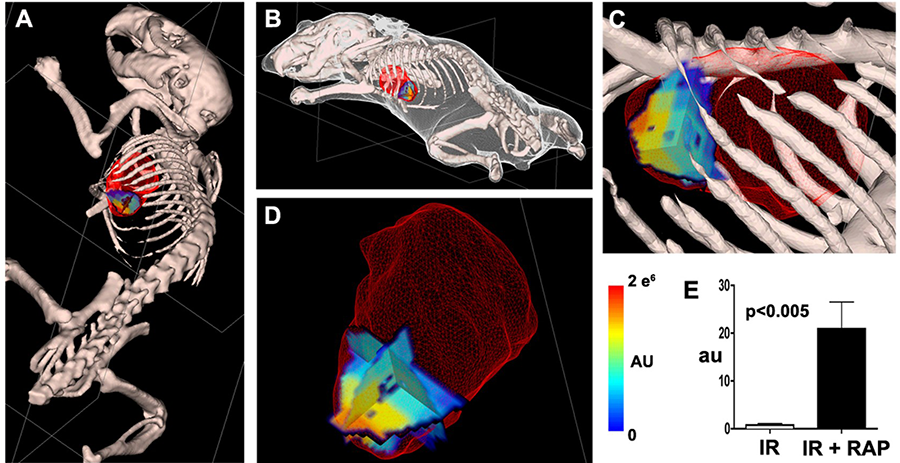
Molecular imaging of cell death, namely autophagy, necrosis, and apoptosis, relies on intravenously injectable contrast agents to target specific biological states and provide sensitive readout. The ability to image cell death processes noninvasively in vivo allows the kinetics to be studied during disease progression and regression. Autophagy is a conserved catabolic process where cells recycle part of the cytoplasm during stress. Interestingly, autophagy can exert both detrimental and protective pathophysiological impacts. We demonstrated for the first time probe-based imaging of autophagy in a beating mouse heart. In mouse hearts with ischemia-reperfusion injury (IR), autophagy induction by Rapamycin (RAP) was visualized and quantified (Figure 1).
Figure 1. Visualizing in vivo cardiac autophagy. (A-D) 3D tomographic fluorescence imaging with an autophagy-sensitive probe in Rapamycin (RAP) treated, ischemia-reperfusion (IR) injured mouse heart. Probe activation is localized to the anterior lateral wall of the heart, consistent with the site of ischemic injury. Fluorescence signal was fused with Computed Tomography (CT) for anatomical coregistration and accurate volumetric quantification (E). n=7 in each cohort, Student’s t-test.
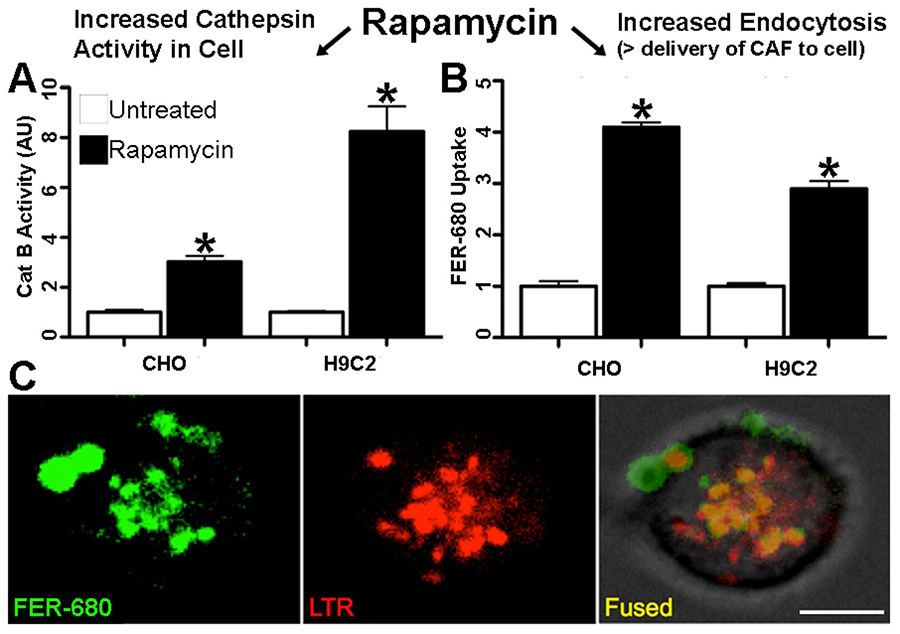
Autophagy imaging probe targets the expanded lysosomal compartment during autophagosome degradation. The probe is specifically activated by lysosomal protease, cathepsin. Autophagy probe uptake mechanism is further elucidated in cell culture (Figure 2). Probe activation following autophagy induction is two-fold: the increased cathepsin activity, the augmented endocytosis of the immediate extracellular space and the subsequent targeting to lysosomes. We hypothesize that bioconjugation chemistry strategies can be applied to engineer second-generation autophagy sensing probes with enhanced cathepsin sensitivity, endocytosis, and lysosomal targeting while preserving specificity.
Figure 2. Activation mechanisms of autophagy-sensing probe. RAP induces autophagy, increasing both cathepsin activity (A) and endocytosis (B). Endocytosed fluorescent nanoparticle (FER-680) is trafficked to the lysosomes, evident by colocalization with lysosomal marker (LTR=lysotracker) in a single cell (C). *p<0.05, ANOVA, triplicates.
Theranostic Nucleic Acid Binding Nanoprobe
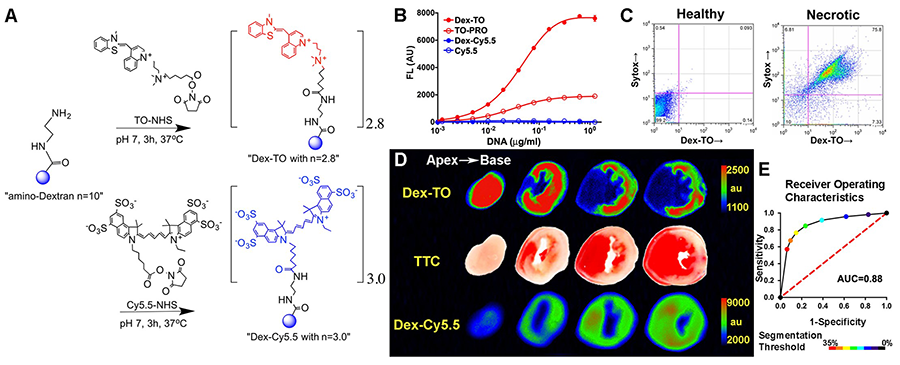
Theranostics are imaging agents with dual therapeutic and diagnostic capabilities. Developing theranostics would allow us to see disease processes non-invasively in the body, simultaneously apply therapeutics at the site of injury, and yield real-time readout of response to treatment. An example of theranostic nanoprobe is a biocompatible polymer construct engineered with nucleic acid chelating fluorochromes. The probe targets nucleic acids released during cell rupture to facilitate imaging of cardiomyocyte necrosis (Figure 3).
Figure 3. Necrosis-sensing optical nanoprobe. (A) Synthesis of the active (Dex-TO) and control (Dex-Cy5.5) probes. (B) Multivalent Dex-TO fluorescence increases robustly with DNA. (C) Dex-TO is excluded from healthy cells, and specifically taken up by necrotic cells. (D) In infarcted mouse heart slices, Dex-TO fluorescence correlates with TTC staining of tissue necrosis. No correlation is seen with control Dex-Cy5.5. (E) Receiver Operating Characteristics of Dex-TO (Area Under the Curve=0.88, n=7 mice).
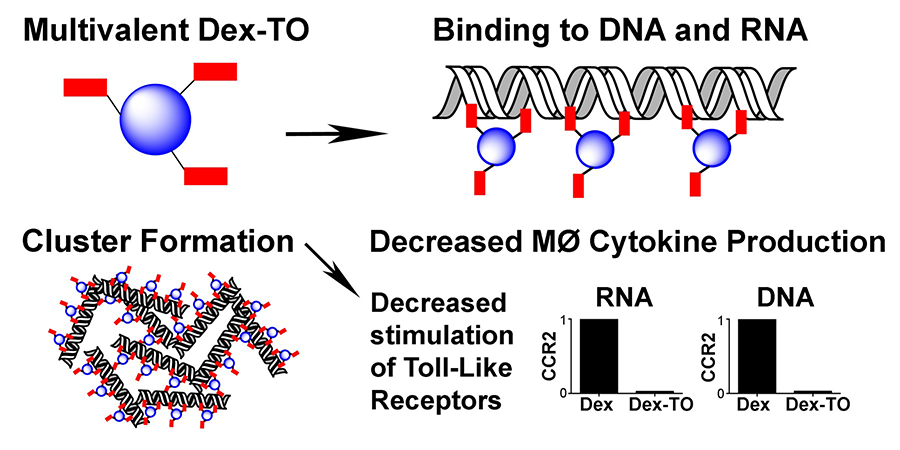
Extracellular nucleic acids are robust proinflammatory molecules that elicit immune cell infiltration. Theranostic nanoprobe developed has nanomolar affinity for mammalian and bacterial nucleic acids, and attenuates the production of inflammatory cytokines from activated macrophages exposed to DNA and RNA (Figure 4). In mice treated with the nanoprobe, inflammation was reduced at 24 hours after myocardial ischemia-reperfusion injury, leading to improved cardiac healing on day 7. Biocompatible polymer platform further allows pharmacokinetics to be optimized to enhance diagnostic and therapeutic efficacies.
Figure 4. Schematics of extracellular nucleic acid chelating nanoprobe to exert anti-inflammatory effects.